"Casi 1/3 de todas las fatalidades en el buceo están asociadas a un evento cardíaco agudo."
El buceo con scuba es una actividad recreativa atractiva para la gente de todas las edades. Aún más, el buceo en condiciones favorables requiere de poco esfuerzo, haciendo fácil que las personas que aún no se han iniciado supongan que es un pasatiempo seguro y natural. Pero es esencial tener en mente que durante cualquier buceo, pueden aparecer condiciones y circunstancias riesgosas que ameriten realizar un gran esfuerzo, prácticamente sin aviso previo.
Sólo la inmersión, ya es un factor generador de stress en el cuerpo, especialmente para el corazón y el sistema circulatorio. Las personas que tienen una capacidad de esfuerzo físico limitado, pueden esforzarse al límite debido al buceo –hasta el punto de una lesión grave, y aún, la muerte. Este capítulo explica algunos datos básicos sobre el corazón en relación al buceo, para ayudarlo a mantenerse seguro y saludable mientras realiza la actividad.
En este capítulo, aprenderá sobre:
- Como el buceo afecta su salud y su sistema circulatorio
- La salud cardíaca y el riesgo de muertemientras bucea
- Comprender el concepto de capacidad de ejercicio aeróbico
- Los efectos del envejecimiento en su sistema cardiovascular
- Calcular la intensidad de la actividad física
- Actividad física recomendaciones
- Poniendo en perspectiva los riesgos y beneficios de la actividad física
Como el buceo afecta su salud y su sistema circulatorio
El buceo con scuba lo expone a muchos efectos que incluyen: la propia inmersión, frío, gases a mayores presiones, elevada presión respiratoria, ejercicio físico y estrés, así como también, al riesgo post buceo de las burbujas de gas circulando por la sangre. La capacidad de su corazón de tolerar un elevado gasto arterial disminuye con la edad y las enfermedades. Tener un corazón sano es de suma importancia para su seguridad mientras bucea así como también para su habilidad para ejercitarse y su expectativa de vida. La información en este cuadernillo está dedicada a ayudarlo a comprender cómo las enfermedades cardíacas pueden afectarlo mientras bucea, y cómo usted puede promover una salud cardíaca óptima.
Los efectos de la inmersión
La inmersión en el agua a una temperatura cercana a la del cuerpo humano, lo expone a un gradiente de presión, que desplaza la sangre de los vasos sanguíneos en sus piernas a los de su cavidad torácica. Esto aumenta el volumen de sangre dentro de su tórax hasta 24 onzas (700mm). Su corazón, entonces, toma entre 6 a 8 onzas (180 a 240 mm) de sangre adicional, que provoca un agrandamiento de las cuatro cámaras del corazón, un aumento de presión en su aurícula derecha, un incremento mayor al 30% de su gasto cardíaco, y un leve aumento de su presión arterial general.
Los baroreceptores (sensores que perciben un cambio en la presión arterial) dentro de los principales vasos sanguíneos de su cuerpo reaccionan a todos estos cambios disminuyendo la actividad de su sistema nervioso simpático, que regula lo que denominamos popularmente la respuesta de "luchar o huír". Como resultado, el ritmo de su corazón disminuye, y la concentración en su plasma sanguíneo de norepinefrina, una hormona del sistema nervioso simpático, decrece; en respuesta a esta caída en la norepinefrina, sus riñones excretan más sodio, y aumenta la producción de orina.
Los efectos del frío
El agua tiene alta conductividad térmica –esto significa que su cuerpo pierde más calor cuando usted está sumergido en agua, que cuando está en aire seco. Usted se siente más cómodo a una temperatura de aire determinada que sumergido en agua a la misma temperatura. Y cuando su cuerpo pierde calor, se intensifica el angostamiento de los vasos sanguíneos periféricos (una condición conocida como "vasoconstricción periférica"). Esto envía más sangre a su corazón, lo que aumenta la presión de llenado en el lado derecho y hace que bombee mayor cantidad de sangre. La constricción de las pequeñas arterias del cuerpo también aumenta la resistencia a la sangre que fluye a través de la periferia de su cuerpo, lo que aumenta su presión arterial, haciendo que su corazón tenga que esforzarse más para mantener un adecuado flujo de sangre a través de todo su cuerpo.
Los efectos de la presión
Respirar aire bajo mayor presión, como usted hace cuando practica buceo con scuba, también afecta su corazón y su sistema circulatorio. Los altos niveles de oxígeno provocan vasoconstricción, aumentan su presión arterial, y reducen su ritmo y su gasto cardíacos. Y los altos niveles de dióxido de carbono – que puede acumularse en el cuerpo cuando usted se ejercita durante un buceo, debido a la ventilación pulmonar reducida causada por los gases densos – pueden aumentar el flujo de sangre a través del cerebro, lo que puede acelerar la toxicidad de oxígeno si usted está respirando una mezcla de gases hiperóxica (con elevado nivel de oxígeno)
Los efectos del ejercicio
El buceo, puede ser físicamente muy exigente, pero los buzos recreativos tienen la opción de elegir las condiciones y actividades de buceo que generalmente no requieren mucho esfuerzo. Sin embargo, cualquier buceo exige cierta demanda de energía metabólica de su cuerpo. Por ejemplo, nadar lenta y relajadamente en la superficie representa una actividad de intensidad moderada (ver Tabla 2 en página …), mientras que nadar con aletas en la superficie requiere hasta un 40% menos energía que hacerlo sin ellas. Pero, al agregar el equipo scuba aumenta la carga en el nadador, y en consecuencia, el gasto de energía al nadar. En 1996, un artículo publicado en Medicine & Science en Sports & Exercise demostró que sólo utilizar un tanque de buceo, puede aumentar el consumo de energía de un buzo en un 25% por sobre la natación regular en superficie a la misma velocidad, y que utilizar un traje seco puede representar otro 25% de aumento en el consumo de energía.
La mayoría de los buceos con flotabilidad neutra y sin corriente sólo requieren de intervalos cortos de nado intermitente a un ritmo lento, y en consecuencia, representan un ejercicio de baja a moderada intensidad. La intensidad del ejercicio se mide en un valor conocido como equivalente metabólico (MET por su sigla en inglés), representando 1 MET la cantidad de energía consumida cuando estamos en reposo. (Ver página…. para una detallada descripción de los cálculos MET). Se sugiere que los buzos pueden mantener el ejercicio a 6 METs durante un período de 20 a 30 minutos. Dado que las personas pueden mantener sólo alrededor del 50% de su capacidad máxima de ejercicio durante un período prolongado, se recomienda que los buzos puedan superar una prueba de esfuerzo a 12 METs.
Los efectos del estrés
Su sistema nervioso autónomo (SNA) – el sistema esencialmente involuntario que regula las funciones internas, tales como sus ritmos cardíaco y respiratorio, y la digestión – también se ve afectado por el buceo. Entre los componentes del SNA se encuentran los sistemas: simpático y parasimpático; mientras el primero regula la respuesta "luchar o huir" de su cuerpo, el sistema parasimpático regula las funciones restantes y ayuda a su cuerpo a conservar la energía. En individuos sanos, bucear generalmente aumenta los efectos parasimpáticos, preservando el ritmo cardíaco, y una medida conocida como variabilidad del ritmo cardíaco. Sin embargo, un buceo que se percibe como estresante, hace que el SNA trabaje en la dirección opuesta, lo que significa que prevalecen los efectos simpáticos, resultando en un incremento del ritmo cardíaco, una disminución en la variabilidad del ritmo cardíaco y un aumento del riesgo de arritmia.
Efectos adversos graves
La mayoría de los efectos que el buceo tiene sobre su corazón y su sistema circulatorio atañe a la capacidad de adaptación de su cuerpo, pero a veces, pueden producirse reacciones adversas graves. Una reacción conocida como bradiarritmia (frecuencia cardiaca muy lenta e irregular) puede provocar la muerte súbita cuando el buzo ingresa al agua, especialmente en individuos con una anomalía del ritmo cardíaco preexistente. Por el contrario, la taquiarritmia (frecuencia cardiaca muy rápida e irregular), también puede provocar la muerte súbita, especialmente en buzos con enfermedad cardiaca estructural o isquémica. Y el esfuerzo excesivo o los efectos del stress pueden sobrecargar al corazón y provocar manifestaciones agudas de enfermedad cardiaca isquémica no diagnosticada previamente.
El buceo en apnea puede, particularmente, provocar efectos cardíacos adversos graves; éstos ocurren en una sucesión rápida en una
respuesta conocida como el "reflejo de buceo". Sus síntomas más significativos incluyen bradicardia (ritmo cardíaco lento),
la reacción vasoconstrictora periférica descripta arriba, y la hipoxia progresiva (falta de una adecuada provisión de
oxígeno). Para evitar el estallido de un pulmón, los buzos con scuba no deben contener la respiración durante el ascenso.

La salud cardíaca y el riesgo de muerte mientras bucea

Las estadísticas muestran que alrededor de un tercio de todas las fatalidades en el buceo están asociadas a un evento cardíaco agudo. En un estudio reciente realizado sobre miembros de DAN, se determinó que la incidencia del total de muertes relacionadas con el buceo es de 16 de cada 100.000 buzos por año, y la de muertes relacionadas con el buceo debido a causas cardíacas es de casi un tercio de ese número -5 de cada 100.000 buzos por año. Debe notarse que el riesgo de muerte relacionada con algún evento cardíaco mientras bucea es 10 veces más alto en buzos mayores de 50 años, que en aquellos menores de esa edad. Aún más, el estudio sobre miembros de DAN mostró un incremento continuo en el riesgo a medida que la edad avanza. Mientras se sospecha que algunos eventos cardíacos pueden estar provocados por actividades o situaciones relacionadas específicamente con el buceo, otros definitivamente no lo están –la muerte súbita también ocurre mientras se encuentra en superficie nadando, o realizando actividades deportivas de diferentes tipos en tierra, y aún mientras descansa o duerme.
Los infartos agudos de miocardio (comúnmente conocidos como "ataques cardíacos") que se producen mientras se realiza un esfuerzo –como nadar contracorriente, con grandes olas, o en condiciones de flotabilidad negativa excesiva- probablemente se encuentren dentro de las fatalidades provocadas por el buceo. Los ataques cardíacos están causados por una provisión insuficiente de sangre a los músculos del corazón; los ataques cardíacos relacionados con el buceo, generalmente ocurren en varones de mediana edad con enfermedad arterial coronaria no diagnosticada.
El buceo (o sólo la inmersión) también puede provocar arritmias agudas, o alteraciones en el ritmo cardíaco, que pueden resultar en muerte súbita. Es más probable que las arritmias provoquen la muerte en buzos mayores. Como explica el Dr. Carl Edmonds en su libro Buceo and Subaquatic Medicine (El Buceo y la Medicina Subacuática), ), y la información de DAN lo confirma, "La víctima a menudo parece tranquila justo antes del colapso final. Algunos estaban inusualmente cansados o descansando, habiendo realizado esfuerzos previamente, o estaban siendo remolcados –lo que sugiere cierto grado de agotamiento. Algunos actuaban como si no se sintieran bien antes del colapso final. Algunos se quejaban de dificultad para respirar sólo unos pocos segundos antes del colapso, mientras otros, bajo el agua, señalaban que necesitaban respirar de su compañero pero rechazaron el regulador que les ofrecieron. Las explicaciones para la disnea incluyen hiperventilación psicogénica, estimulación de la respiración autonómica, y edema pulmonar –este último demostrado en la autopsia. En todos los casos hubo una adecuada provisión de aire disponible, lo que sugiere que su disnea no estaba relacionada con problemas del equipo. Algunas víctimas perdieron el conocimiento sin haberles hecho ninguna señal a su compañero, mientras otros pidieron ayuda de manera tranquila"
La incidencia de muerte súbita (MS) también aumenta con la edad. Los patrones de MS son similares entre los buzos, y entre la población general; sin embargo, es importante que los buzos no desestimen la posibilidad de una relación causal entre el buceo y la MS. Casos de MS donde no hubo un factor externo obvio que la provocara, ocurren con mayor frecuencia en buzos mayores. Los exámenes post mortem realizados a víctimas de MS, revelan signos de enfermedad cardiaca previamente no sospechada más que un evento específico que la precipitó. La mejor forma de evitar la MS es, en consecuencia, prevenir la enfermedad cardiaca, y mantener el buen estado físico a medida que su edad avanza.
Comprender el concepto de capacidad de ejercicio aeróbico

Su capacidad para la actividad física sostenida depende de la cantidad de energía que su cuerpo puede producir en un proceso utilizando oxígeno, y se denomina capacidad aeróbica. Su capacidad aeróbica individual depende de qué tan bien funcione su sistema cardiovascular –corazón y vasos sanguíneos. Es el sistema que mueve su sangre a través de sus pulmones, donde se carga de oxígeno, y luego la distribuye a cada parte de su cuerpo, donde el oxígeno sostiene la vida, alimenta sus músculos, y estimula su habilidad para realizar ejercicios. El "motor" del sistema circulatorio es el corazón. Es una bomba hecha de tejido vivo: músculos, tejido conectivo, y un sistema conductor que produce señales eléctricas que estimulan la acción de bombeo de su corazón. Un corazón vació pesa un promedio de poco más de media libra (250 a 300 gr) en mujeres, y entre dos tercios y tres cuartos de libra (300 a 350 gr) en varones. Tiene cuatro cámaras: la aurícula derecha, el ventrículo derecho, la aurícula izquierda, y el ventrículo izquierdo.
Las aurículas reciben sangre a baja presión. La derecha recibe sangre venosa que regresa al corazón desde todo el cuerpo ya carente de oxígeno. La aurícula izquierda recibe sangre que regresa al corazón desde los pulmones luego de haber sido nuevamente enriquecida con oxígeno. Los ventrículos realizan la mayor parte del bombeo. El derecho bombea sangre hacia y a través de los pulmones, mientras el izquierdo mantiene la circulación de sangre a través de todo el cuerpo, hacia sus órganos y tejidos. La sangre fluye a través del corazón, sólo en una dirección, gracias a un sistema de válvulas que se abren y cierran en el momento exacto. Cuán fuerte y/o rápido tiene que trabajar su corazón depende de muchos factores, incluso su nivel de actividad.
En promedio, un corazón humano bombea alrededor de 2.4 onzas (70 mm) de sangre por latido –una medida que se conoce como "volumen sistólico o de bombeo"
El corazón de un individuo en reposo late, en promedio, 72 veces por minuto (ésta es su frecuencia cardiaca), que resulta en un gasto cardíaco según se señala a continuación:
- 1.3 galones (5 litros) de sangre por minuto
- 1900 galones (7200 litros) por día
- 700'000 galones (2628000 litros) por año
- 48 millones de galones (184 millones de litros) a lo largo de un vida promedio de 70 años.
Y ese gasto es sólo para satisfacer las necesidades metabólicas básicas del cuerpo en reposo: aproximadamente 3.5 mililitros de oxígeno por kilogramo de masa corporal por minuto. Este índice metabólico en reposo se indica como un equivalente metabólico, expresado como "1 MET". Cuando usted realiza ejercicios, los músculos de su cuerpo requieren más oxígeno, por eso su flujo sanguíneo aumenta para satisfacer esa necesidad; su frecuencia cardiaca puede triplicarse, y su volumen sistólico o de bombeo puede duplicarse. Esto incrementa el gasto cardíaco de una persona en buen estado físico promedio desde alrededor de 1.3 galones (5 litros) por minuto hasta entre 4 y 5 galones (15 a 20 litros) por minuto, y en un atleta de alto rendimiento hasta 10 galones (40 litros) por minuto. Y no sólo aumenta el flujo sanguíneo, sino que también más oxígeno se extrae de cada unidad de sangre. Como resultado de estos cambios, el nivel metabólico de una persona de buen estado físico promedio ejercitándose a su capacidad máxima aumenta hasta aproximadamente 12 METs, y en un atleta de alto rendimiento corriendo a un ritmo de 4.17 millas (ó 22.5 kilómetros) por hora, puede aumentar hasta 23 METs.
Los efectos del envejecimiento en su sistema cardiovascular
La habilidad de un individuo de sostener un alto nivel de ejercicio físico durante un prolongado período disminuye con la edad, aunque se encuentre sano. Esta disminución puede ser más lenta si se ejercita regularmente, pero no puede evitarse por completo. Es provocada por un debilitamiento de las funciones de todos los sistemas del cuerpo, aunque el foco aquí, está puesto en el corazón.
El corazón tiene un sistema de ritmo que controla los latidos y regula las señales eléctricas que estimulan la acción de bombeo que realiza. Con el paso del tiempo, este marcapasos natural pierde algunas de sus células, y pueden dañarse algunas de sus vías eléctricas. Estos cambios pueden resultar en una frecuencia cardiaca levemente más lenta en reposo, y una mayor susceptibilidad a los ritmos anormales (el más común conocido como "fibrilación auricular")
A mayor edad, todas las estructuras del corazón también se ponen más rígidas. Los músculos del ventrículo izquierdo se engrosan, el corazón puede aumentar levemente su tamaño, y el volumen del ventrículo izquierdo puede disminuir. Como resultado, el corazón puede llenarse y vaciarse más lentamente, poniendo, en consecuencia, menos sangre en circulación. El aumento en la frecuencia y el gasto cardíaco en respuesta a la actividad física también disminuye, como también la frecuencia cardiaca máxima. Esta caída de la frecuencia cardiaca máxima parece ser mayor que la promedio en individuos sedentarios y en aquellos con enfermedad cardiovascular evidente.
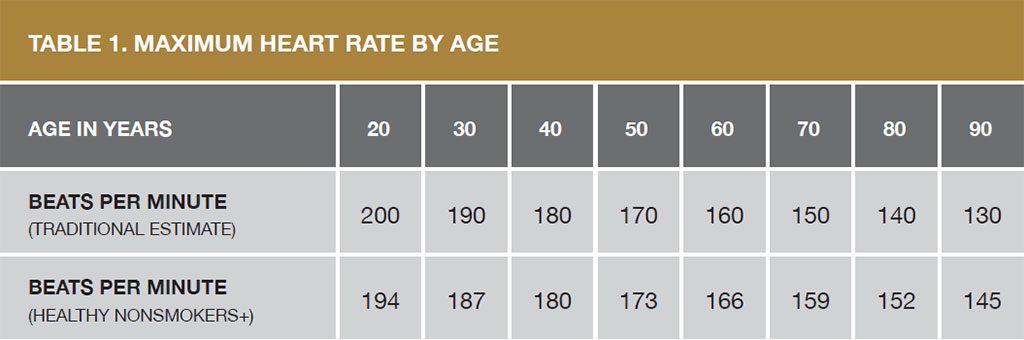
+ Tanaka y algunos coautores propusieron una fórmula actualizada en 2001 para no fumadores sanos, de 208 menos 7/10 de la edad del individuo.
Source: Modificada de "Age-predicted maximal heart rate revisited" by H. Tanaka H et al. Journal of the American College of Cardiology; 2001; Volumen. 37; páginas 153-156.
El sistema nervioso autónomo también cambia con la edad. Generalmente, su componente parasimpático establece el nivel de frecuencia cardiaca en reposo, mientras su componente simpático regula al corazón en anticipación de y en respuesta a la actividad física –estimulando un oportuno y apropiado aumento en el flujo sanguíneo para mantener la actividad. Los continuos ajustes entre los sistemas simpático y parasimpático resultan en pequeñas variaciones de la frecuencia cardiaca (un factor conocido como "variabilidad de la frecuencia cardiaca") que son evidentes sobre una base de latido-a-latido –el tipo de regulación sensible que es marca distintiva de un sistema de control saludable. A medida que la edad avanza, sin embargo, la contribución del sistema parasimpático disminuye; la actividad del sistema simpático aumenta, aún en reposo, la variabilidad de la frecuencia cardiaca desaparece, y el ritmo cardíaco se vuelve más propenso a las interrupciones. Esta caída de la variabilidad de la frecuencia cardiaca relacionada con la edad, y el aumento en del ritmo cardíaco en reposo (debido a la disminución de la actividad del parasimpático) son responsables de un aumento de 2.6 veces en el riesgo de MS.
Calcular la intensidad de la actividad física
La intensidad de cualquier actividad física puede calcularse directamente — midiendo la cantidad de oxígeno que usted utiliza para metabolizar la energía (un valor que se abrevia VO2, por "volumen de oxígeno") por minuto de ejercicio — o indirectamente — midiendo su frecuencia cardíaca y utilizando ese valor como un índice del esfuerzo que está poniendo en su corazón y sus pulmones.
Medición directa de la Intensidad del Ejercicio
La cantidad de energía que usted utiliza en cualquier momento es proporcional a la cantidad de oxígeno que su cuerpo requiere. En reposo, una persona sana promedio utiliza aproximadamente 3.5 milímetros de oxígeno por kilogramo de peso corporal por minuto; esto se conoce como "frecuencia metabólica en reposo". El gasto de energía de una actividad física puede expresarse como múltiplo de una frecuencia metabólica en reposo; esto se conoce como "equivalente metabólico de la tarea", o simplemente equivalente metabólico, y se abrevia MET.
Un individuo en buen estado físico promedio puede lograr una frecuencia metabólica aproximadamente 12 veces mayor (lo que se expresa como "12 METs"), mientras que los atletas de alta competición pueden exceder un nivel de 20 METs
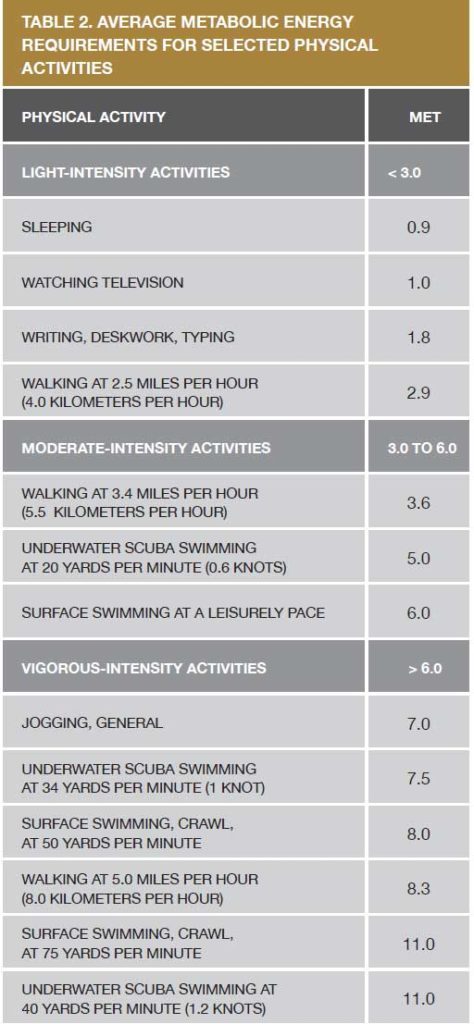
La tabla de la derecha muestra ejemplos de actividades clasificadas como de intensidad leve, moderada, o vigorosa, basadas en la cantidad de energía requerida para realizarlas.
Fuente: "Compendium of physical activities: an update of activity codes and MET intensities"; "Oxygen consumption in underwater swimming"; y "Oxygen uptake studies of divers when fin swimming with maximum effort at depths of 6–176 feet" (vea "Lecturas adicionales y fuentes" para más detalles de esta fuente).
La capacidad aeróbica máxima de un individuo se expresa como la mayor absorción de oxígeno mientras se ejercita al máximo (lo que se abrevia como "VO2 max"). Medir la VO22 con precisión requiere seguir estrictos protocolos en un laboratorio de fisiología y desempeño deportivos — procedimiento conocido como "prueba de ejercicio máximo". Realizar dichas pruebas lleva mucho tiempo y es muy costoso, por eso sólo se utilizan en situaciones especiales.

Estimación indirecta de la Intensidad del Ejercicio
También es posible realizar un estimado relativo de la intensidad de una actividad midiendo sus efectos sobre las frecuencias cardíacas y respiratorias. Esto puede realizarse de varias maneras.
El test del habla: Si una persona sana promedio puede hablar pero no cantar mientras se está ejercitando, esa actividad se considera de moderada intensidad. Una persona que está realizando una actividad de intensidad vigorosa no puede decir más que unas pocas palabras sin hacer una pausa para tomar aire. Si usted debe esforzarse para tomar aire y no puede hablar durante lo que generalmente se considera un ejercicio de intensidad moderada, significa que su capacidad física está por debajo del promedio.
El test de la frecuencia cardiaca: su frecuencia cardiaca aumenta de manera regular a medida que la intensidad de su actividad se incrementa (aunque la frecuencia cardiaca máxima que usted puede lograr disminuirá con la edad). Usted puede calcular la frecuencia cardiaca máxima promedio para individuos sanos de su edad, restando su edad a 220. Por ejemplo, la frecuencia cardiaca máxima para una persona de 50 años se calcularía de la siguiente manera: 220 – 50 = 170 latidos por minuto (lpm). Entonces, usted puede utilizar su frecuencia cardiaca real para estimar la intensidad relativa de varias actividades que realiza, y para, indirectamente, calcular su capacidad de ejercicio máximo. Los expertos a menudo recomiendan alcanzar y sostener una determinada frecuencia cardiaca para mejorar o mantener el buen estado físico.
Prueba de ejercitación sub-máxima: Una prueba de ejercitación sub-máxima puede utilizarse para calcular su capacidad de ejercitación máxima sin exceder el 85% de la frecuencia cardiaca máxima estimada para su edad. Realizar dicha prueba requiere que se aumente gradualmente la intensidad del ejercicio, basado en un protocolo definido, mientras se monitorea su frecuencia cardiaca. Cuando usted alcanza la frecuencia cardiaca propuesta como meta, se detiene el ejercicio y su capacidad de ejercitación máxima puede entonces extrapolarse utilizando varios métodos. Sin embargo, a causa de las variaciones en la relación entre la frecuencia cardiaca y la intensidad del ejercicio debido a la edad, al nivel de estado físico y a otros factores, una estimación indirecta de la capacidad aeróbica máxima tiene un valor limitado. No obstante, la prueba aún tiene valor como herramienta clínica para evaluar la tolerancia de un individuo para realizar ejercicios y, la probabilidad de sufrir una enfermedad cardiaca isquémica.
Actividad física recomendaciones
Los adultos necesitan dos tipos de actividades regulares para mantener o mejorar su salud –entrenamiento aeróbico y de fuerza. Las normas sobre la actividad física de los Centros de Control y Prevención de Enfermedades del año 2008 para los norteamericanos recomiendan al menos, dos horas y media por semana de ejercicio aeróbico de intensidad moderada para lograr beneficios para la salud, y cinco horas por semana para lograr beneficios adicionales para el buen estado físico. Y tan importante como realizar ejercicios aeróbicos es hacer actividades para el fortalecimiento muscular, por lo menos dos días por semana.
Las actividades físicas se clasifican generalmente, según su nivel de intensidad en una de estas cuatro categorías:
- COMPORTAMIENTO SEDENTARIO: se refiere a actividades que no aumentan sustancialmente la frecuencia cardíaca o el gasto de energía por sobre el nivel del reposo; se incluyen en esta categoría actividades como dormir, estar sentado, recostarse, y ver televisión. Tales actividades implican un gasto de energía de 1,0 a 1,5 METs.
- ACTIVIDAD FÍSICA DE INTENSIDAD LEVE: este tipo de actividad — a menudo agrupada dentro de las de comportamiento sedentario, es en realidad, un nivel de actividad diferente- implica un gasto de energía de entre 1.6 a 2.9 METs y eleva la frecuencia cardiaca a menos del 50 % de la frecuencia cardiaca máxima. Se incluyen dentro de este tipo de actividades caminar lentamente, el trabajo administrativo, cocinar y lavar los platos.
- ACTIVIDAD FÍSICA DE MODERADA INTENSIDAD: es aquella que incrementa la frecuencia cardiaca hasta entre el 50% y el 70% de la frecuencia cardiaca máxima. Por ejemplo, las personas de alrededor de 50 años tienen una frecuencia cardiaca máxima estimada en 170 latidos por minuto (lpm), entonces los niveles del 50% y del 70% serían de 85 lpm y 119 lpm. Esto significa que una actividad de intensidad moderada para personas de 50 años es aquella que mantiene su frecuencia cardiaca entre 85 lpm y 119 lpm. En comparación, las personas de alrededor de 30 años tienen una frecuencia cardiaca máxima estimada de 190 lpm, siendo para ellas una actividad de intensidad moderada aquella que eleve su frecuencia cardiaca hasta entre 95 lpm y 133 lpm.
- ACTIVIDAD FÍSICA DE INTENSIDAD VIGOROSA: es aquella que aumenta la frecuencia cardiaca hasta entre el 70% y 85% de la frecuencia cardiaca máxima. Para las personas mayores de 60 años, esto sería entre 122 lpm y 136 lpm; para las de 25 años, entre 136 lpm y 167 lpm.
Pueden encontrarse recomendaciones detalladas sobre la actividad física en cdc.gov/physicalactivity/everyone/guidelines (en inglés).

Chequeo previo a realizar actividad física
Realizar actividad física es beneficioso para la salud, pero pasar de un estilo de vida sedentario a estar físicamente activo, o aumentar el nivel usual de actividad, puede asociarse con un riesgo mayor –especialmente en individuos con enfermedades cardíacas pre-existentes. El buceo con scuba, generalmente, implica actividad física de intensidad moderada, pero pueden aparecer situaciones que requieran de actividad de alta intensidad. Además, el buceo con scuba desafía al sistema cardiovascular de varias maneras, lo que puede ser potencialmente peligroso para la salud de las personas con enfermedad cardiaca o con baja capacidad para el ejercicio.
Una herramienta común de revisión previa a realizar actividades es La Declaración Médica del Consejo de Entrenamiento de Buceo Recreativo (RSTC). Este cuestionario lo interroga tanto sobre su historial médico, como también sobre síntomas y signos de enfermedades crónicas y agudas. Si los potenciales buzos padecen cualquiera de las condiciones que aparecen en la lista, se les aconseja consultar a un médico para realizarse una evaluación de su estado físico para bucear. La mayoría de los operadores de buceo utilizan el formulario RSTC para checar a sus clientes, y si usted marca cualquier condición que necesita evaluación médica, pero no puede presentar documentación que acredite un examen médico reciente que lo habilite a bucear, pueden impedírselo. Por eso, usted debería completar dicho formulario antes de realizar cualquier viaje durante el que planee bucear y, si fuese necesario, obtener una evaluación por escrito de un médico que conozca sobre medicina del buceo –y llevarlo en el viaje.
Y recuerde que es de suma importancia que usted sea honesto al completar el cuestionario. Usted tiene las llaves para una participación segura en cualquier actividad física, incluso el buceo con scuba.
Además, independientemente de su condición médica, se les aconseja a los hombres mayores de 45 años, y a las mujeres mayores de 50, que controlen su salud anualmente con su médico de cabecera. Y todos los buzos con cualquier factor de riesgo de enfermedad cardiaca deberían ver a su médico de cabecera antes de comenzar a bucear, y asegurarse de seguir cualquier consejo que reciban.
Poniendo en perspectiva los riesgos y beneficios de la actividad física

En general, realizar una actividad física regularmente reduce el riesgo de muerte de un individuo por enfermedad cardiaca –pero en personas susceptibles, la actividad intensa puede aumentar el riesgo de un infarto agudo de miocardio (ataque al corazón) o de muerte súbita (MS). Las personas con ateroesclerosis avanzada –un desorden que genera un angostamiento de las arterias debido a la formación de depósitos de grasa en sus paredes internas –son especialmente susceptibles a tales riesgos.
La incidencia de infarto agudo de miocardio y MS es mayor en individuos generalmente sedentarios, especialmente los que comienzan a realizar una actividad física a la que no están acostumbrados. Un artículo publicado en el New England Journal of Medicine Medicine reveló que los hombres habitualmente sedentarios tenían 56 veces más probabilidades de morir, durante o luego de ejercitarse intensamente que el resto; en comparación, los hombres físicamente muy activos sólo tenían cinco veces más probabilidades de morir durante o después de realizar actividad física intensa que el resto. Otro artículo del New England Journal of Medicine informó que el infarto agudo de miocardio era 50 veces más probable durante o inmediatamente después de realizar ejercicio físico intenso en los sujetos menos activos que en los más activos.
Por eso, mientras se les aconseja a los individuos sedentarios modificar su estilo de vida y ejercitarse regularmente –comenzando con actividades de baja intensidad, e incrementando gradualmente la misma – puede ser que requieran un chequeo antes de comenzar. Los individuos con cualquier limitación de salud necesitan tanto autorización médica como, preferentemente, un entrenador profesional. Las personas con alto riesgo de sufrir enfermedades cardíacas deberían abstenerse de realizar ciertas actividades. Para mayor información, lea "Cuándo consultar a un profesional de la salud antes de comenzar a realizar actividades físicas".
Es importante enfatizar, sin embargo, que hasta las prácticas más restrictivas nunca prevendrán por completo los eventos cardiovasculares asociados con el ejercicio. Es entonces esencial que los individuos que realizan ejercicios reconozcan e informen los síntomas que, a menudo, preceden a un evento cardíaco; se conocen como "síntomas prodrómicos", y pueden incluir uno o más de los siguientes:
- Dolor de pecho (conocido como "angina de pecho)
- Fatiga en aumento
- Indigestión, acidez, u otro problema gastrointestinal
- Excesiva falta de aire
- Dolor de oído o cuello
- Sensación de malestar general
- Infecciones del tracto respiratorio alto
- Mareos, palpitaciones, o dolor de cabeza severo
Se ha demostrado que tales síntomas estuvieron presentes en el 50% de los corredores, el 75% de los jugadores de squash, el 81% de los fondistas, y el 60% de los buzos con scuba que murieron mientras realizaban ejercicio. La gente que realiza actividad física debe conocer estos hechos, y los médicos deberían interrogar a los pacientes durante los exámenes médicos sobre sus hábitos de ejercicio y el conocimiento que tienen sobre los síntomas prodrómicos. Los buzos que experimenten cualquiera de los síntomas descriptos arriba cuando están ejercitándose, deberían realizarse una evaluación médica antes de retomar la actividad.
Siguiente: Capítulo 2 - Factores de riesgo de la enfermedad cardiovascular