“Nearly 1/3 of all diving fatalities are associated with an acute cardiac event.”
Scuba diving is an appealing recreational activity for people of all ages. Indeed, diving in favorable conditions requires little exertion, making it easy for the uninitiated to assume that diving is a safe and effortless pastime. But it is essential to keep in mind that during any dive, perilous conditions and circumstances can arise that may call for vigorous exercise on a moment’s notice.
Immersion alone is a stressor on the body, especially the heart and circulatory system. People who have limited exercise capacity may be pushed to their limit by diving — to the point of serious injury and even death. This chapter explains some basic information about the heart in relation to diving to help keep you safe and healthy as you dive.
In this chapter, you’ll learn about:
- How Diving Affects Your Health and Circulatory System
- Cardiac Health and Your Risk of Death While Diving
- Understanding the Concept of Aerobic Exercise Capacity
- The Effects of Aging on Your Cardiovascular System
- Calculating Physical Activity Intensity
- Physical Activity Recommendations
- Placing the Risks and Benefits of Physical Activity in Perspective
How Diving Affects Your Health and Circulatory System
Scuba diving exposes you to many effects, including immersion, cold, hyperbaric gases, elevated breathing pressure, exercise and stress, as well as a postdive risk of gas bubbles circulating in your blood. Your heart’s capacity to support an elevated blood output decreases with age and with disease. Having a healthy heart is of the utmost importance to your safety while scuba diving, as well as to your ability to exercise generally and your life span. The information in this booklet is devoted to helping you understand how heart disease can affect you while you’re diving and how you can promote optimal heart health.
Effects of Immersion
Immersion in water near the temperature of the human body exposes your body to a pressure gradient, which shifts blood from the vessels in your legs to those in your chest cavity. This increases the volume of blood within your chest by up to 24 ounces (700 milliliters). Your heart thus takes in an additional 6 to 8 ounces (180 to 240 milliliters) of blood, resulting in an enlargement of all four chambers, an increase in pressure in your right atrium, a more than 30-percent increase in cardiac output and a slight increase in your overall blood pressure.
Baroreceptors (sensors that perceive a change in blood pressure) within your body’s major vessels react to all these changes by decreasing the activity of your sympathetic nervous system, which governs what’s popularly called the “fight-or-flight” response. As a result, your heart rate declines and the concentration in your plasma of norepinephrine, a hormone of the sympathetic nervous system drops; in response to the drop in norepinephrine, your kidneys excrete more sodium, and your urine production increases.
Effects of Cold
Water has high thermal conductivity—that is, your body loses more heat when you’re immersed in water than when you’re in dry air. You’ll feel more comfortable at a given air temperature than when you’re immersed in water of the same temperature. And when your body loses heat, that intensifies the narrowing of your peripheral blood vessels (a condition known as “peripheral vasoconstriction”). This in turn sends more blood to your heart, which increases the filling pressure on the right side of your heart and makes it pump more blood. Constriction of the body’s small arteries also increases the resistance to blood flowing through the periphery of your body, which raises your blood pressure, meaning your heart has to exert itself more to maintain an adequate flow of blood throughout your body.
Effects of Pressure
Breathing air under increased pressure, as you do when scuba diving, also affects your heart and circulatory system. Increased levels of oxygen cause vasoconstriction, increase your blood pressure and reduce your heart rate and heart output. And increased levels of carbon dioxide—which may accumulate in the body when you exercise during a dive, due to reduced pulmonary ventilation caused by dense gases—can increase the flow of blood through your brain, which can speed up oxygen toxicity if you’re breathing a hyperoxic gas mix (one with an elevated level of oxygen).
Effects of Exercise
Diving can be very physically demanding, but recreational divers have the option of choosing diving conditions and activities that typically do not require a lot of exertion. Nevertheless, any dive places some metabolic energy demands on your body. For example, slow, leisurely swimming on the surface represents a moderate-intensity activity (see Table 2 on page 11), while swimming with fins on the surface requires up to 40 percent less energy than barefoot swimming. But the addition of scuba equipment increases drag on the swimmer and thus the energy cost of swimming. A 1996 paper in the journal Medicine & Science in Sports & Exercise showed that wearing just one scuba tank may increase a diver’s energy consumption by 25 percent over regular surface swimming at the same speed, and that using a drysuit may result in another 25 percent increase in energy consumption.
Most dives at neutral buoyancy and with no current require only short intervals of intermittent swimming at a slow pace and thus represent low-to-moderate intensity exercise. Exercise intensity is measured by a value known as metabolic equivalent (MET), with 1 MET representing the amount of energy consumed when at rest. (See page 11 for a detailed description of MET calculations.) It is suggested that divers be able to sustain exercise at 6 METs for a period of 20 to 30 minutes. Since people can sustain only about 50 percent of their peak exercise capacity for a protracted period, it is recommended that divers be able to pass an exercise stress test at 12 METs.
Effects of Stress
Your autonomic nervous system (ANS)—the largely involuntary system that regulates internal functions, such as your heart rate, respiratory rate and digestion—is affected by diving, too. Among the components of the ANS are the sympathetic and parasympathetic systems; while the sympathetic system governs your body’s “fight-or-flight” response, the parasympathetic system governs resting functions and helps your body conserve energy. In healthy individuals, diving generally increases parasympathetic effects, preserving the heart rate and a measure known as heart rate variability. A dive that is perceived as stressful, however, pushes the ANS in the other direction, meaning sympathetic effects prevail—resulting in an increase in the heart rate, a decline in heart rate variability and an increase in the risk of arrhythmia.
Serious Adverse Effects
Most of the effects that diving has on your heart and circulatory system fall within your body’s capacity to adapt, but sometimes serious adverse reactions can occur. A reaction known as bradyarrhythmia (a very slow and irregular heartbeat) can cause sudden death upon a diver’s entry into the water, especially in individuals with a preexisting rhythm anomaly. Conversely, tachyarrhythmia (a very rapid and irregular heartbeat) can also cause sudden death, especially in divers with structural or ischemic heart disease. And overexertion or the effects of stress may strain the heart and result in acute manifestations of previously undiagnosed ischemic heart disease.
Breath-hold diving can have particularly serious adverse cardiac effects; these effects occur in quick succession in a
response known as the “diving reflex.” Its most significant elements include bradycardia (a slowing of the heart rate);
the peripheral vasoconstriction reaction described above; and progressive hypoxia (or lack of an adequate supply of
oxygen). To avoid bursting a lung, scuba divers must not hold their breath during ascent.

Cardiac Health and Your Risk of Death While Diving

Statistics show that about one-third of all diving fatalities are associated with an acute cardiac event. In a recent study of DAN members, the incidence of diving-related deaths overall was determined to be 16 per 100,000 divers per year, and of diving-related deaths due to cardiac causes, to be nearly a third of that number—5 per 100,000 divers per year. It is of particular note that the risk of cardiac-related death while diving is 10 times higher in divers over age 50 than in those under 50. Indeed, the study of DAN members showed a continuous increase in risk with increasing age. While some suspected cardiac events may be provoked by dive-specific activities or situations, other cardiac events may not be caused by a dive at all—inasmuch as sudden cardiac death also occurs while engaged in surface swimming or land-based sporting activities of various sorts and even while at rest or during sleep.
Acute myocardial infarctions (commonly known as “heart attacks”) that are brought on by exertion — such as while swimming against a current, in heavy waves or under conditions of excessive negative buoyancy — are likely involved in some dive-provoked fatalities. Heart attacks are caused by an insufficient blood supply to the muscles of the heart; diving-related heart attacks typically occur in middle-aged males with undiagnosed coronary artery disease.
Diving (or just immersion) may also provoke acute arrhythmias, or disturbances of the heart’s rhythm, that can likewise result in sudden death. Arrhythmias are more likely to cause death in older divers. As Dr. Carl Edmonds explains in his book Diving and Subaquatic Medicine, and DAN data confirms, “The victim often appeared calm just before his final collapse. Some were unusually tired or resting, having previously exerted themselves, or were being towed at the time—suggesting some degree of exhaustion. Some acted as if they did not feel well before their final collapse. Some complained of difficulty in breathing only a few seconds before the collapse, whereas others underwater signaled that they needed to buddy breathe, but rejected the offered regulator. Explanations for the dyspnea include psychogenic hyperventilation, autonomic induced breathing stimulation and pulmonary edema—the latter being demonstrated at autopsy. In all cases there was an adequate air supply available, suggesting that their dyspnea was not related to equipment problems. Some victims lost consciousness without giving any signal to their buddy, whereas others requested help in a calm manner.”
The incidence of sudden cardiac death (SCD) also increases with age. Patterns of SCD are similar among divers and among the general population; nevertheless, it is important that divers not dismiss the possibility of a causative relationship between diving and SCD. Cases of SCD where there was no obvious external provoking factor occur more frequently in older divers. Postmortem examinations of SCD victims are more likely to reveal signs of previously unsuspected heart disease than a specific precipitating event. The best way to prevent SCD is thus to prevent heart disease and to maintain physical fitness and wellness as you age.
Understanding the Concept of Aerobic Exercise Capacity

Your capacity for sustained physical activity depends on the amount of energy your body can produce in a process using oxygen called aerobic capacity. Your individual aerobic capacity depends on how well your cardiovascular system—your heart and blood vessels—works. It’s the system that moves your blood through your lungs, where it’s loaded with oxygen, and then distributes it to every part of your body, where the oxygen sustains life, nourishes your muscles and supports your ability to exercise. The “motor” of the circulatory system is the heart. The heart is a pump made of live tissue: muscles, supportive tissue and a conduction system that produces the electrical signals which stimulate your heart’s pumping action. An empty heart weighs an average of a little over half a pound (250 to 300 grams) in females and between two-thirds and three-quarters of a pound (300 to 350 grams) in males. It has four chambers: the right atrium, right ventricle, left atrium and left ventricle.
The atria receive blood at low pressure. The right atrium receives venous blood returning to the heart from all over the body after it’s been depleted of oxygen. The left atrium receives blood returning to the heart from the lungs after it’s been enriched again with oxygen. The ventricles do most of the pumping. The right ventricle pumps blood to and through the lungs, while the left ventricle maintains the circulation of blood throughout the body, to all its organs and tissues. Blood flows through the heart in only one direction, thanks to a system of valves that open and close at just the right time. How hard your heart has to work varies depending on many factors, including your activity level.
On average, a human heart pumps about 2.4 ounces (70 milliliters) of blood per heartbeat—a measure that’s known as “stroke volume.”
The heart of an individual at rest beats, on average, 72 times per minute (this is your “heart rate”), which results in a cardiac output as follows:
- 1.3 gallons (5 liters) of blood per minute.
- 1,900 gallons (7,200 liters) per day.
- 700,000 gallons (2,628,000 liters) per year.
- 48 million gallons (184 million liters) over an average life span of 70 years.
And that output is just to meet the body’s basic metabolic needs at rest: about 3.5 milliliters of oxygen per kilogram of body mass per minute. This resting metabolic rate is designated as one metabolic equivalent, which is expressed as “1 MET.” When you exercise, your body’s muscles require more oxygen, so your blood flow increases to meet that need; your heart rate may increase threefold and your stroke volume may double. This increases the cardiac output of a person of average fitness from about 1.3 gallons (5 liters) per minute to between 4 and 5 gallons (15 and 20 liters) per minute, and of a top athlete to as much as 10 gallons (40 liters) per minute. And not only does the blood flow increase, but more oxygen is extracted from each unit of blood. As a result of these changes, the metabolic level of a person of average fitness exercising at peak capacity increases to about 12 METs, and of a top athlete running a 4:17 mile (or a 22.5-kilometers-per-hour pace) may increase to 23 METs.
The Effects of Aging on Your Cardiovascular System
An individual’s ability to sustain a high level of exercise for a prolonged period of time decreases with age, even with healthy aging. This decline can be slowed by regular exercise, but it cannot be avoided completely. The decline is caused by a weakening of the functions of all the body’s systems, though the focus here is on the heart.
The heart has a pacing system that controls the heartbeat and regulates the electrical signals that stimulate the heart’s pumping action. Over time, this natural pacemaker loses some of its cells, and some of its electrical pathways may get damaged. These changes can result in a slightly slower heart rate at rest and a greater susceptibility to abnormal rhythms (the most common of which is known as “atrial fibrillation”).
With increasing age, all the structures of the heart also become more rigid. The muscles of the left ventricle get thicker, the heart may increase slightly in size and the volume of the left ventricle may decline. As a result, the heart may both fill and empty more slowly, thus putting less blood into circulation. The increase in one’s heart rate and cardiac output in response to physical activity is also diminished, and one’s maximum heart rate declines. The drop in maximum heart rate appears to be greater than average in sedentary individuals and in those with overt cardiovascular disease.
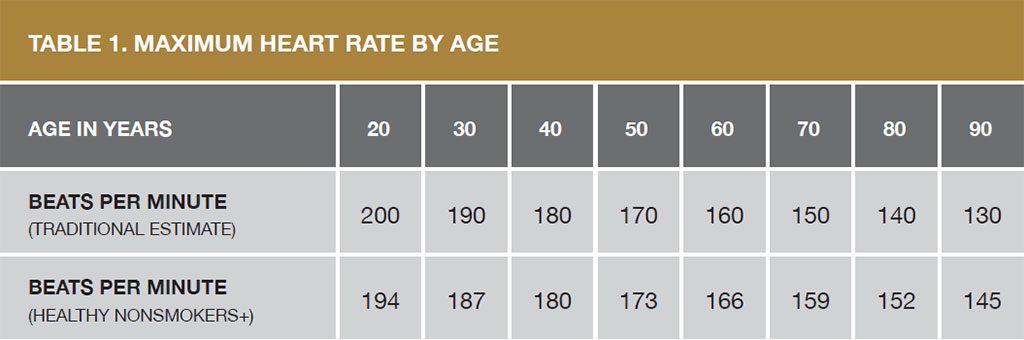
+ Tanaka and coauthors proposed an updated formula in 2001 for healthy nonsmokers of 208 less 7/10ths of the individual’s age.
Source: Modified from “Age-predicted maximal heart rate revisited” by H. Tanaka H et al. Journal of the American College of Cardiology; 2001; Vol. 37; pages 153-156
The autonomous nervous system changes with age, too. Normally, its parasympathetic component sets the level of the heart rate at rest, while its sympathetic component governs the heart in anticipation of and in response to physical activity—stimulating a timely and appropriate increase in blood flow to support the activity. Continuous adjustments between the sympathetic and parasympathetic systems result in minute variations in the heart rate (a factor known as “heart rate variability”) that are evident on a beat-to-beat basis—the kind of sensitive regulation that is a signature of a healthy control system. With increasing age, however, the contribution of the parasympathetic system wanes; the sympathetic system’s activity increases, even at rest; heart rate variability disappears; and the heart’s rhythm becomes more prone to disruption. This age-related falloff in heart rate variability and increase in resting heart rate (due to the decline in parasympathetic activity) are responsible for a 2.6-fold increased risk of SCD.
Calculating Physical Activity Intensity
The intensity of any physical activity can be calculated directly—by measuring the amount of oxygen you use for energy metabolism (a factor that’s abbreviated as VO2, short for “volume of oxygen”) per minute of exercise—or indirectly—by measuring your heart rate and using that value as an index of the strain your exertion is placing on your heart and lungs.
Direct Measurement of Exercise Intensity
The amount of energy you use at any given time is proportional to the amount of oxygen your body requires. At rest, the average healthy person uses roughly 3.5 milliliters of oxygen per kilogram of body weight per minute; this is known as “resting metabolic rate.” The energy cost of a physical activity can be expressed as a multiple of resting metabolic rate; this is known as “metabolic equivalent of task,” or simply metabolic equivalent, and is abbreviated as MET.
An individual of average fitness can achieve about a 12-fold increase in metabolic rate (which is expressed as “12 METs”), while top athletes can exceed a 20-MET increase.
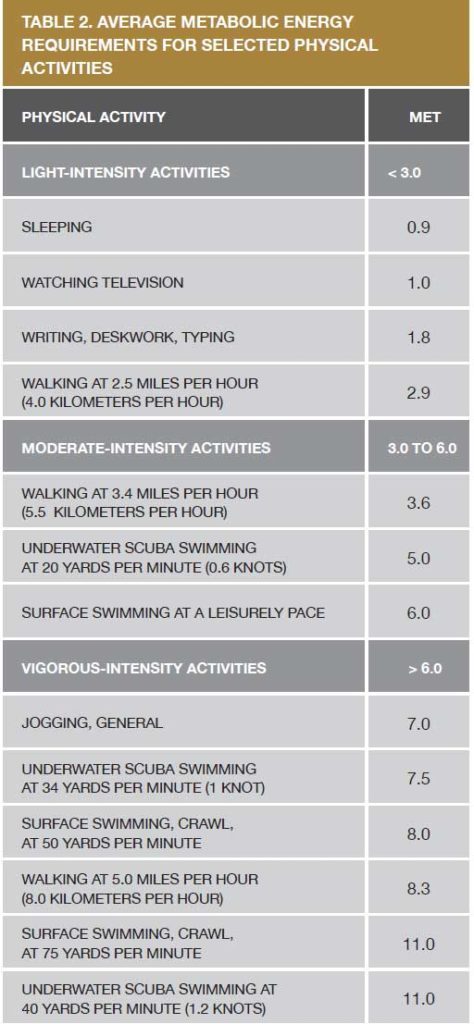
The table to the right lists examples of activities classified as being of light, moderate or vigorous intensity, based on the amount of energy required to do them.
Sources: “Compendium of physical activities: an update of activity codes and MET intensities”; “Oxygen consumption in underwater swimming”; and “Oxygen uptake studies of divers when fin swimming with maximum effort at depths of 6–176 feet” (see the list of further readings on page 53 for details on these sources).
An individual’s peak aerobic capacity is expressed as maximum oxygen uptake while engaged in all-out exercise (which is abbreviated as “VO2 max”). Measuring VO2 max accurately requires following strict protocols in a sports-performance lab – a procedure known as a “maximal exercise test.” Conducting such tests is time-consuming and expensive, so they are used only in special situations.

Indirect Estimation of Exercise Intensity
It is also possible to make a relative estimate of an activity’s intensity by measuring its effects on your heart rate and respiration rate. This can be done in several ways.
Talk test: If an average healthy person can talk but not sing while exercising, that activity is considered to be of moderate intensity. A person engaged in vigorous-intensity activity is not able to say more than a few words without pausing for a breath. If you must gasp for air and cannot talk during what is generally considered to be moderate-intensity exercise, it means that your physical capacity is below average.
Heart rate test: Your heart rate rises in a regular fashion as the intensity of your activity increases (though the maximum heart rate you’re able to achieve will decline as you age). You can figure the average maximum heart rate for healthy individuals your age by subtracting your age from 220. For example, the maximum heart rate for a 50-year-old would be calculated as follows: 220 – 50 = 170 beats per minute (bpm). You can then use your actual heart rate to estimate the relative intensity of various activities you engage in and to indirectly estimate your maximum exercise capacity. Experts often recommend reaching and sustaining a certain heart rate to improve or maintain fitness.
Submaximal exercise test: A submaximal exercise test can be used to figure your maximum exercise capacity without exceeding 85 percent of the estimated maximum heart rate for your age. Conducting such a test calls for gradually increasing your exercise intensity, based on a defined protocol, while your heart rate is being monitored. When you reach the target heart rate, you stop exercising and your maximum exercise capacity can then be extrapolated using various methods. However, because of variations in the relationship between heart rate and exercise intensity due to age, fitness level and other factors, an indirect estimation of maximum aerobic capacity has limited value. Nevertheless, the test is still a valuable clinical tool to assess an individual’s tolerance for exercise and likelihood of having ischemic heart disease.
Physical Activity Recommendations
Adults need two types of regular activity to maintain or improve their health—aerobics and strength training. The Centers for Disease Control and Prevention’s 2008 Physical Activity Guidelines for Americans recommends at least two and a half hours a week of moderate-intensity aerobic exercise to achieve health benefits, and five hours a week to achieve additional fitness benefits. And just as important as engaging in aerobic exercise is doing muscle-strengthening activities at least two days a week.
Physical activities are commonly classified by intensity into one of the following four categories:
- SEDENTARY BEHAVIOR: Sedentary behavior refers to activities that do not substantially increase one’s heart rate or energy expenditure above the resting level; included in this category are activities like sleeping, sitting, lying down and watching television. Such activities involve an energy expenditure of 1.0 to 1.5 METs.
- LIGHT-INTENSITY PHYSICAL ACTIVITY: Light physical activity—which is often grouped with sedentary behavior but is, in fact, a distinct activity level—involves an energy expenditure of between 1.6 and 2.9 METs and raises the heart rate to less than 50 percent of one’s maximum heart rate. It encompasses such activities as slow walking, deskwork, cooking and washing dishes.
- MODERATE-INTENSITY PHYSICAL ACTIVITY: Physical activity that increases the heart rate to between 50 percent and 70 percent of one’s maximum heart rate is considered to be of moderate intensity. For example, 50-year-olds have an estimated maximum heart rate of 170 beats per minute (bpm), so the 50-percent and 70-percent levels would be 85 bpm and 119 bpm. That means a moderate intensity activity for 50-year-olds is one that keeps their heart rate between 85 bpm and 119 bpm. By contrast, 30-year-olds have an estimated maximum heart rate of 190 bpm, making a moderate-intensity activity one that raises their heart rate to between 95 bpm and 133 bpm.
- VIGOROUS-INTENSITY PHYSICAL ACTIVITY: A vigorous-intensity activity is one that increases the heart rate to between 70 percent and 85 percent of one’s maximum heart rate. For 60-year-olds, that would be between 122 bpm and 136 bpm; for 25-year-olds, it would be between 136 bpm and 167 bpm.
Detailed physical activity recommendations can be found at cdc.gov/physicalactivity/everyone/guidelines.

Pre-Activity Screening
Engaging in physical activity is beneficial for one’s health, but making the transition from a sedentary lifestyle to being physically active, or increasing one’s accustomed level of activity, may be associated with increased risk—especially in individuals with preexisting heart disease. Scuba diving typically involves moderate intensity physical activity, but situations can occur that require high-intensity activity. In addition, scuba diving challenges the cardiovascular system in a variety of ways that may be life-threatening for individuals with heart disease or a low capacity for exercise.
A common pre-activity screening tool is the Recreational Scuba Training Council (RSTC) Medical Statement and Guidelines. The RSTC questionnaire asks about your medical history, as well as symptoms and signs of chronic and acute diseases. If prospective divers have any of the listed conditions, they are advised to consult with a physician to obtain a medical evaluation of their fitness to dive. Most dive operators use the RSTC form to screen customers, and if you check any conditions that call for medical evaluation but cannot present documentation of a recent exam that has cleared you for diving, you may be unable to dive. So you should complete the RSTC Medical Statement in advance of any trip during which you plan to dive and, if necessary, obtain a written evaluation from a physician knowledgeable about diving medicine—and take it with you on your trip.
And remember that it is of the utmost importance that you be honest in filling out the questionnaire: You hold the keys to your safe participation in any physical activity, including scuba diving.
In addition, regardless of their medical condition, men age 45 and older and women age 50 and older are advised to review their health annually with their primary-care physician. And all divers with any risk factors for cardiac disease should see their primary-care physician before engaging in diving and should be sure to follow any advice they’re given.
Placing the Risks and Benefits of Physical Activity in Perspective

In general, engaging in regular physical activity reduces an individual’s risk of death due to heart disease—but in susceptible individuals, vigorous activity can increase the risk of an acute myocardial infarction (heart attack) or of sudden cardiac death (SCD). Individuals with advanced atherosclerosis—a disorder that involves a narrowing of the arteries due to a buildup of fatty deposits on their inner walls—are especially susceptible to such risks.
The incidence of both acute myocardial infarction and SCD is greatest in generally sedentary individuals, especially those who engage in unaccustomed physical activity. A paper published in the New England Journal of Medicine found that habitually sedentary men were 56 times more likely to experience cardiac death during or after vigorous exercise than when at rest; by contrast, very physically active men were only five times more likely to die during or after vigorous exercise than when at rest. Another New England Journal of Medicine paper reported that an acute myocardial infarction was 50 times more likely during or soon after vigorous physical exercise in the least active than in the most active subjects.
So while sedentary individuals are advised to change their lifestyle and take up regular physical exercise—starting with low-intensity activities and gradually increasing the intensity at which they exercise—they may require pre-activity screening. Individuals with any health limitations need both medical clearance and, preferably, a professional fitness coach. Individuals identified as being at high risk for cardiac problems should abstain from certain activities. For relevant guidelines, read “When to consult a health-care provider before engaging in physical activities.”
It is important to emphasize, however, that even the most restrictive practices will never be able to completely prevent cardiovascular events associated with exercise. It is thus essential that individuals who exercise recognize and report the symptoms that often precede a cardiac event; these are known as “prodromal symptoms” and may include one or more of the following:
- Chest pain (known as “angina”).
- Increasing fatigue.
- Indigestion, heartburn or other gastrointestinal symptoms.
- Excessive breathlessness.
- Ear or neck pain.
- A feeling of vague malaise.
- Upper respiratory tract infections.
- Dizziness, palpitations or a severe headache.
Such symptoms have been shown to be present in 50 percent of joggers, 75 percent of squash players, 81 percent of distance runners and 60 percent of scuba divers who die while exercising. People who exercise must be aware of these facts, and physicians should query patients during medical exams about their exercise habits and their knowledge of prodromal symptoms. Divers who experience any of the symptoms above during exercise should obtain a medical evaluation before they resume diving.