Helping Divers Dive Longer, Deeper, and Safer
Pieter-Jan van Ooij, MD, PhD, is the head of the Department of Research, Innovation, and Education at the Royal Netherlands Navy’s Diving Medical Centre (DMC). As the Netherlands’ leading facility for diving and dive medicine for armed forces divers, the DMC also helps professional and civilian divers who need medical advice.
Van Ooij plans and initiates dive research to determine how divers can dive longer, deeper, and safer.
What is your educational background, and how did you become interested in this field?
After graduating in 1991, I considered pursuing a career in either anesthesiology or respiratory medicine. Getting specialized training in these fields was very challenging in the Netherlands at the time, however, so I started working in cardiology as a nontraining resident.

One day I read a newspaper interview with Rob van Hulst, who was head of the DMC. I had always been interested in diving, so I thought, “What could be better than a combination of diving and medicine?” Instead of entering the navy, I decided to train to be an occupational physician and then merge into dive medicine.
After finishing my training in 1998, I worked at a commercial occupational health center before joining the Royal Netherlands Army’s occupational health center in 2000. In 2002 I was appointed as the army’s dive medical physician. The DMC was already the center of expertise in dive medicine, so van Hulst and I decided to combine dive medical care for both forces. In 2006 I started at the DMC as a civilian dive medical physician and have remained there since.
Tell us about your research on pulmonary oxygen toxicity markers.
During my doctoral studies on pulmonary oxygen toxicity, I primarily aimed to identify a better marker for its development during diving. My supervisor was respiratory physiologist Peter Sterk, who was producing promising results on volatile organic compounds (VOCs) in asthma, chronic obstructive pulmonary disease (COPD), lung cancer, and tuberculosis patients.
That success inspired us to see if VOCs were relevant in dive medicine. I found five relevant VOCs, most of which were alkanes and methyl alkanes. Other researchers found similar results, indicating that we had found a correlation with pulmonary oxygen toxicity, although we need additional research for a final confirmation.
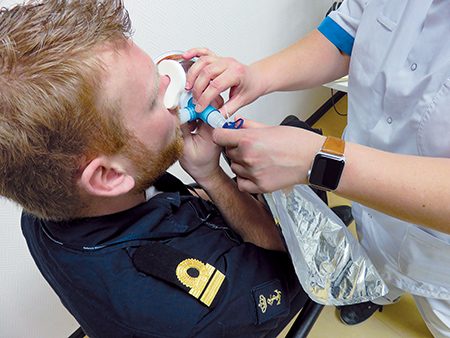
Our focus going forward is on the use of electronic noses (e-noses) once we gather enough data. E-noses use a gas sensor and convert gas molecular signals from exhaled breath into electric signals, giving those signals an identity. The alcohol breath test that law enforcement officers use is one example. Our goal is to make the device smaller and pair it with an app that can indicate dive readiness with a simple color-coded system. This system holds a lot of potential for enhancing the safety of dive operations, particularly for special forces, who require extended, deeper, and safer dives. This will be my primary project for the next couple of years.
Some physicians outside of dive medicine question the use of hyperoxia. Have you encountered fears of hyperoxia in your work?
During my initial research on pulmonary oxygen toxicity, I needed approval from the medical-ethical committee at the University of Amsterdam, where some anesthesiologists questioned administering 100% oxygen based on fears of oxygen-related complications in intensive care units.
In the late 1960s, many people with compromised respiratory systems got worse after long periods of being intubated with 100 percent oxygen. The older ventilator models delivered only a fraction (40% to 50%) of the supplied oxygen to patients, but new devices deliver much more.
Our research suggests that administering higher concentrations of oxygen, up to 100% if necessary, can be beneficial for patients, especially in improving white blood cell function and patient recuperation. Even with our findings, some medical professionals still have a lingering apprehension about hyperoxia. Recognizing the caution stems from the history of oxygen therapy, we encourage tailoring oxygen levels to meet the patients’ needs.
You have also investigated health differences in submariners. What did you find?
We looked at the well-being of retired submariners and how their unique living conditions impacted their mental and physical health. Factors such as prolonged absence of sunlight, lack of privacy, and the submarine environment can have significant effects on individuals. Exploring these elements could give us insight into developing new submarines and evaluating crew working hours and shift schedules.
Our findings from a questionnaire sent to retired submariners showed that they generally reported better overall health than their civilian peers. The questionnaire was broad in scope, with questions including how they felt, how frequently they visited a physician, and their drinking habits. We did not ask for specific health issues such as heart or lung problems. The occupational medicine department of the Netherlands Ministry of Defense is following up by further investigating these aspects and going deeper into submariners’ health, including lung health and cancer risk.
Tell us about your project involving antihistamines and nitrogen narcosis.

That study looked at the effects of old- and new-generation antihistamine medications on nitrogen narcosis. Participants were administered three different medications (old generation, new generation, and placebo) on separate dives, one medication per dive, without knowing the medication type. They then took reactivity tests at depths of 0 feet, 33 feet (10 meters), and 98 feet (30 meters). We found that the nitrogen narcosis levels induced by the new-generation antihistamine were comparable to those the placebo induced, showing that it does not influence nitrogen narcosis. We determined the new-generation antihistamine is safe for dives up to 98 feet (30 meters).
My participation in this study came from wanting to see the procedure as a participant and show our other participants that we were not conducting any unusual procedures. I could tell from my experience which medication was the old generation, as it made me incredibly drowsy. Like the other participants, I could not distinguish the effects of the new-generation medication and the placebo. Everyone could identify the old-generation medication, because it made them drowsy as well.
There is not much research about medications in diving in general. I understand why after the challenges we had obtaining approval from a medical-ethical committee for this study. I hope people will continue this line of research because while using medications may not strictly disqualify someone from diving, it is important to recognize the potential risks. The greater concern is the underlying disease causing the diver to take the medication rather than the medication and its side effects.
You come from the occupational medicine side and have done thousands of fitness-to-dive evaluations. What is your opinion on chest X-rays in fitness-to-dive exams for commercial diving?
Some of our current research focuses on fitness to dive, and the procedures haven’t changed in a long time. We recently conducted a study examining whether an audiometry test is necessary for divers and asking if they should be performed annually, especially considering its absence in recreational dive standards.
We also looked into the benefit of taking chest X-rays, which comes from the 1960s, when high-resolution computed tomography (HRCT) was not yet developed. Chest X-rays were the best option for detecting tuberculosis-related lung damage at that time, but they may now be obsolete.
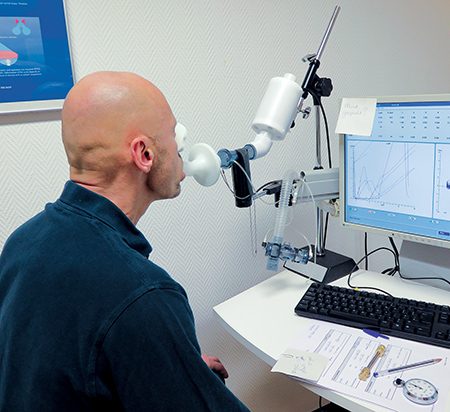
We did a retrospective study looking at the differences in detecting pulmonary anomalies from both chest X-rays and HRCT. We found that HRCT was more accurate in finding anomalies such as bullae, although it can present other findings as well, such as renal abnormalities. We concluded that a very good questionnaire and thorough medical history are sufficient for assessing a diver’s health status, including pulmonary health. If doctors suspect anything from that information, then they can do an HRCT or a chest X-ray if HRCT is not available. We stopped doing chest X-rays in the Dutch navy and hope that more naval and occupational medicine institutions will follow that lead.
What do you expect the future of dive medicine to look like?
Over the next 50 years I anticipate significant changes in dive research and technology. Artificial intelligence and electronics developments will make things that seem impossible today feasible. Scuba gear may look very different or even be obsolete due to advancements.
Personalized dive systems that account for temperature, sweat, gas consumption, bubble formation, and other factors could eliminate the need for standardized dive tables. With potential environmental challenges such as climate change, underwater habitats may become more popular.
While we may not have artificial gills or fully integrated dive systems yet, ongoing research will make progress like that possible.
© Alert Diver — Q2 2024