SAYA TELAH MENJADI PENYELAM BERSERTIFIKAT sejak 1986 dan telah mencatat ratusan penyelaman rekreasi dan teknis. Sejak 2014 saya terutama melakukan penyelaman rebreather teknis dengan sekelompok penyelam rebreather berpengalaman dari California Utara.
During the summer of 2019, our group visited Lake Huron’s Thunder Bay National Marine Sanctuary in Michigan to dive the historic shipwrecks from the late 1800s that rest nearly intact in 160 to 200 feet of icy cold and clear fresh water. Emmy-Award-winning underwater cinematographer and technical diving instructor Becky Kagan Schott and her husband, David Schott, who is also an accomplished cameraman and technical diver, organized our trip. We spent the months before the trip doing workup dives in Lake Tahoe, where water conditions are similar to Lake Huron’s.
Our Lake Huron dive plans included two dives per day, all of which entailed mandatory decompression stops because of the depth and time we spent exploring each shipwreck. As I descended the mooring line, my eyes strained for the first glimpse of what was on the bottom. I passed through the thermocline and into the clear 39°F water until I saw a narrow, dark object slowly come into view at 80 feet. It was the top of a still-upright mast. Goosebumps rose on my skin as the entirety of the wooden schooner revealed itself in nearly 100 feet of visibility. With such intact ships and artifacts, these wrecks were as close as I could get to a trip through time.

Di tengah perjalanan, saya mulai merasa gatal di sekitar dada saya di bawah pakaian selam saya selama interval permukaan. Saya langsung merasa tidak enak, karena ini adalah ketiga kalinya saya merasakan sensasi ini dalam lima tahun. Saya membuka baju saya dan melihat tanda-tanda kulit yang melengkung: Benjolan merah, bernoda, dan meninggi yang mengindikasikan penyakit dekompresi kulit (DCS) menutupi bagian dada kiri atas saya. Saya segera memberi tahu Becky tentang hal itu dan mulai menghirup oksigen 100 persen melalui alat bantu pernapasan sambil berbaring dan beristirahat di atas kapal. Rasa gatal dan ruam mereda dalam waktu 30 menit.
Ketika berbicara dengan Becky dan Dave tentang situasi saya malam itu, Dave bertanya apakah saya telah menjalani pemeriksaan foramen ovale paten (PFO). Ayahnya, seorang ahli jantung, telah mengatakan kepada Dave bahwa DCS yang berulang kali merupakan indikasi untuk memeriksa PFO. Sebuah lubang kecil di antara dua bilik jantung bagian atas memungkinkan darah mengalir dari atrium kanan ke atrium kiri saat Anda berada di dalam rahim, tetapi setelah Anda lahir dan bernapas sendiri, lubang tersebut secara alami menyatu bagi kebanyakan orang. Namun, pada sekitar 25 persen populasi, lubang tersebut tetap terbuka sebagian, tetapi biasanya tidak menimbulkan efek buruk. Meskipun risiko DCS secara keseluruhan rendah, risiko ini lebih tinggi pada penyelam yang memiliki PFO.
I contacted DAN and sent them my computer logs, but there was nothing remarkable about my dive profiles. I have always been diligent about my hydration, and on this dive I had extended my final decompression stop beyond my already conservative decompression schedule. Thanks to DAN, I started to educate myself about PFOs, and my circumstances aligned with having one. DAN’s medical staff recommended that I have a bubble contrast test.
Dokter layanan primer saya, yang tidak memiliki pengalaman dengan PFO dan menyelam, merujuk saya ke ahli jantung. Dalam beberapa minggu, saya menjalani pemeriksaan kontras gelembung, yang melibatkan penyuntikan jarum suntik larutan garam dan gelembung udara ke dalam pembuluh darah lengan untuk melewati sistem sirkulasi saya sambil melakukan USG jantung. Saya tidak perlu menunggu hasil pemeriksaan, karena saya dapat melihat dengan jelas ketika gelembung-gelembung tersebut melewati atrium saya melalui PFO. Saya merasa lega karena memiliki jawaban potensial atas misteri seputar serangan kulit saya yang melengkung, sementara rekan-rekan penyelam saya yang melakukan profil penyelaman yang sama tidak mengalami efek buruk seperti itu.
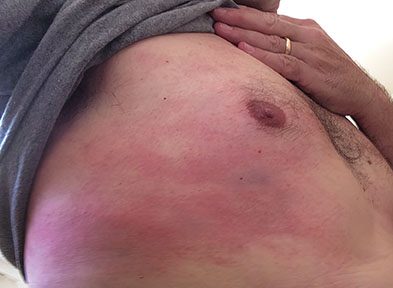
Foto oleh Keith C. Flood
Setelah tes, saya dirujuk ke dokter bedah jantung berpengalaman yang mengkhususkan diri dalam penutupan PFO. DAN mendampingi saya di setiap langkah untuk memastikan bahwa saya berada di jalur yang benar untuk membuat keputusan yang tepat tentang apakah akan menutup PFO saya. Saya khawatir tentang kemungkinan berhenti menyelam, menyelam hanya untuk rekreasi di kedalaman yang dangkal, atau menjalani prosedur medis elektif untuk menutup lubang di jantung saya.
Setelah berbicara dengan beberapa penyelam lain yang kembali menyelam setelah menjalani prosedur penutupan PFO, berkonsultasi dengan DAN, dan menimbang pro dan kontra dengan tim medis saya, saya memilih untuk menutup PFO saya.
Prosedur ini dilakukan dengan menggunakan anestesi lokal saat jantung Anda masih membuat Anda tetap hidup. Dokter bedah memasukkan alat penutup yang terbuat dari nikel dan titanium melalui kateter dari pembuluh darah besar di kaki ke jantung. Kadang-kadang prosedur ini dapat dilakukan dengan rawat jalan, tetapi prosedur saya termasuk rawat inap semalam di rumah sakit. Enam bulan setelah penutupan, tes kontras gelembung tindak lanjut memastikan PFO ditutup secara permanen, dan saya diizinkan untuk kembali menyelam.
I worked back up to how I was diving before my PFO closure, but I still pay close attention to all the best practices for technical diving. I always stay hydrated, dive conservative profiles, add some time to my final decompression stop, and never hesitate to pass on a dive if things just don’t feel right.