DAN® medical information specialists and researchers answer your dive medicine questions.
SAYA BARU SAJA MENJALANI OPERASI OTAK. Operasi itu berhasil, tetapi sekarang bagian tengkorak saya telah diganti dengan jaring. Dokter bedah saraf saya sangat ahli, tetapi tidak tahu bagaimana operasi tersebut dapat memengaruhi penyelaman saya. Apakah saya masih bisa menyelam? Haruskah saya membatasi diri pada kedalaman tertentu, atau haruskah saya hanya snorkeling?
Meskipun operasi Anda berhasil, kembali menyelam setelah jenis operasi ini mungkin atau mungkin tidak dapat dilakukan. Mengizinkan seseorang untuk menyelam setelah operasi otak adalah proses yang rumit, dan setiap orang perlu dinilai berdasarkan kasus per kasus. Setelah operasi otak apa pun, ada periode pemulihan minimum yang harus Anda amati sebelum mempertimbangkan untuk menyelam karena risiko kejang yang meningkat. Kejang di lingkungan bawah air sering kali berakibat fatal, dan peningkatan risiko aktivitas kejang merupakan kontraindikasi mutlak untuk menyelam.
Seperti yang Anda sebutkan, dokter bedah Anda mungkin tidak terbiasa dengan penyelaman dan pengobatan selam. Kami secara teratur menyediakan konsultasi untuk dokter dan mendorong penyedia layanan medis untuk menghubungi kami secara individual untuk mendiskusikan pertanyaan mereka. Kami dengan senang hati memberikan informasi dan rekomendasi sehingga dokter Anda dapat membuat keputusan yang tepat tentang kebugaran Anda untuk menyelam.
- Ben Strelnick, NREMT, W-EMT
Saya lahir sekitar dua bulan sebelum waktunya. Retinopati prematuritas adalah komplikasi utama, dan saya menjalani oksigen, krioterapi, dan gesper sklera sebagai pengobatan. Saya ingin mencoba menyelam. Apakah ada yang harus saya khawatirkan?
No studies that we are aware of suggest that diving is contraindicated in individuals who have had retinopathy of prematurity. It is important to ensure that at least two months have passed since the surgery and that there is no iatrogenic gas bubble in your eye — retinal surgeons sometimes inject those to facilitate healing after surgery. They remain present for varying lengths of time, depending on the gas the surgeon uses. Residual gas in the eye is an absolute contraindication to diving. It sounds as though none of these considerations apply in your case.

Retinopati adalah masalah utama dalam menyelam. Jika bidang penglihatan Anda sangat terpengaruh, hal ini dapat menyebabkan Anda tidak dapat membaca alat pengukur atau merespons situasi yang memerlukan perhatian segera. Seorang penyelam harus dapat melakukan hal berikut:
- Baca alat pengukur yang menunjukkan tekanan udara, kedalaman, waktu menyelam, dan persyaratan dekompresi
- Membaca kompas
- Menemukan dan menavigasi titik masuk dan keluar
- Temukan dan kenali teman mereka
Kami menyarankan Anda untuk memberitahukan niat Anda untuk menyelam kepada dokter mata sebagai bagian dari proses mendapatkan izin medis untuk menyelam.
—Anne Strysniewicz, AEMT, DMT
I was getting back into diving after a few years off when I was diagnosed with primary myelofibrosis. I have asked my doctors about it, and while they know the disease, I do not think they know about diving’s physiological effects. What concerns should I have about diving?
Seperti yang Anda ketahui, mielofibrosis adalah kanker langka yang menyerang sumsum tulang. Sumsum tulang bertanggung jawab untuk memproduksi sel-sel yang membantu tubuh kita mempertahankan kondisi teratur yang dikenal sebagai homeostasis. Sel-sel ini termasuk sel darah merah yang membawa oksigen dan faktor pembekuan darah yang disebut trombosit. Anda mungkin perlu memperhatikan beberapa hal saat memutuskan apakah Anda sehat untuk menyelam.
Gangguan pada produksi sel darah merah dapat menyebabkan anemia, yang dapat bermanifestasi sebagai kelemahan fisik, kelelahan, atau sesak napas. Menyelam adalah aktivitas fisik yang melelahkan dari awal hingga akhir, termasuk mengangkut tangki dan perlengkapan, mengenakan dan melepas perlengkapan di atas kapal, berenang melawan arus, dan memanjat tangga sambil mengenakan perlengkapan. Pengerahan tenaga ini mungkin berbahaya bagi Anda, dan Anda harus mempertimbangkan risiko yang dapat ditimbulkannya bagi orang lain jika Anda membutuhkan penyelamatan. Mudah mengalami pendarahan atau memar juga perlu dipertimbangkan karena kemungkinan penurunan sel darah tertentu. Pendarahan ringan akibat jatuh, gendang telinga yang pecah atau berlubang, atau barotrauma dapat menjadi lebih parah dan menyebabkan masalah pendarahan.
The level of your condition’s malignancy may put you at a greater risk of opportunistic infections, neuropathy, pericardial effusion, and other factors that can lead to convulsions underwater or pulmonary barotrauma.
Efek dan efek samping dari obat apa pun yang Anda minum adalah pertimbangan lebih lanjut. Meskipun obat-obatan memetabolisme atau berpotensi lebih cepat di lingkungan hiperbarik, Anda harus mempertimbangkan bagaimana obat tersebut membuat Anda merasa. Obat pereda nyeri dapat memiliki sifat narkotika atau menimbulkan efek penenang, yang dapat sangat memengaruhi pemikiran kognitif Anda dan cara Anda merespons kejadian yang tidak terduga.
Jika Anda mengonsumsi obat untuk mengobati kondisi Anda, efek sampingnya dapat berupa mual dan muntah. Beberapa tanda dan gejala yang mungkin Anda alami mirip dengan penyakit dekompresi dan menyulitkan diagnosis. Untuk perjalanan menyelam, Anda juga harus mengetahui akses ke perawatan darurat di lokasi Anda jika diperlukan.
We can’t determine if you should or should not dive, but we can educate you about the risks you may encounter. Please review this information with your physician along with the RSTC Medical Statement to determine your fitness to dive.
— Robert Soncini, NR-P, DMT

Sekitar enam minggu yang lalu, saya melakukan manuver Valsava untuk membersihkan telinga setelah turun dari pesawat dan menyadari ada udara yang keluar dari sudut dalam mata kanan saya, sepertinya dari saluran air mata. Sejak saat itu, saya dapat merasakan embusan udara keluar dari tempat itu setiap kali saya membuang ingus. Saya tidak memiliki gejala lain, tetapi apakah ini sesuatu yang perlu dikhawatirkan saat saya menyelam?
Apa yang Anda gambarkan, tampaknya merupakan udara yang melewati saluran nasolakrimal ketika meniup hidung atau mencoba menyamakannya dengan menggunakan manuver Valsava. Fenomena ini tidak jarang terjadi, dan sebagian orang mengalaminya ketika mereka mencoba menyamakannya dengan terlalu paksa. Anda mungkin melakukan manuver Valsava dengan terlalu kuat. Ekualisasi seharusnya merupakan proses yang lembut dan mudah dengan sedikit usaha.
Meskipun mungkin terasa aneh atau sedikit menggelitik, Anda seharusnya tidak mengalami masalah apa pun setelah menyelam. Ada kemungkinan infeksi akibat memaksa lendir dari saluran hidung masuk ke dalam saluran nasolakrimal.
Kami sarankan untuk berkonsultasi dengan dokter spesialis telinga, hidung, dan tenggorokan (THT) setempat tentang masalah Anda. Pengetahuan tentang kedokteran selam tidak diperlukan karena ini adalah masalah umum yang terjadi pada banyak orang, termasuk yang bukan penyelam.
- Ben Strelnick, NREMT, W-EMT
Baru-baru ini saya mengalami serangan jantung yang disebabkan oleh stres, dan dokter saya mendiagnosis saya dengan sindrom Takotsubo. Elektrokardiogram menunjukkan fungsi jantung saya kembali normal, dan ahli jantung saya mengharapkan pemulihan penuh. Langkah apa yang harus saya ambil, dan apa yang harus saya waspadai sebelum menyelam lagi?
Kardiomiopati Takotsubo, atau sindrom patah hati, disebabkan oleh stres atau emosi yang kuat dan dapat sembuh seiring berjalannya waktu. Meskipun gejalanya mungkin tampak seperti serangan jantung, patofisiologinya sangat berbeda.
In a conventional heart attack, a blockage forms at a site of narrowing arteries. This blockage impacts oxygen flow to the heart and can cause infarction (tissue death). With Takotsubo, there is often a lessened blood flow but not a complete blockage, resulting in reduced oxygen to the muscle. Electrocardiograms and blood tests may indicate the patient has suffered a heart attack, but the cardiologist can see no evidence of a blockage. Takotsubo often results in the heart’s left ventricle being enlarged and not working properly.
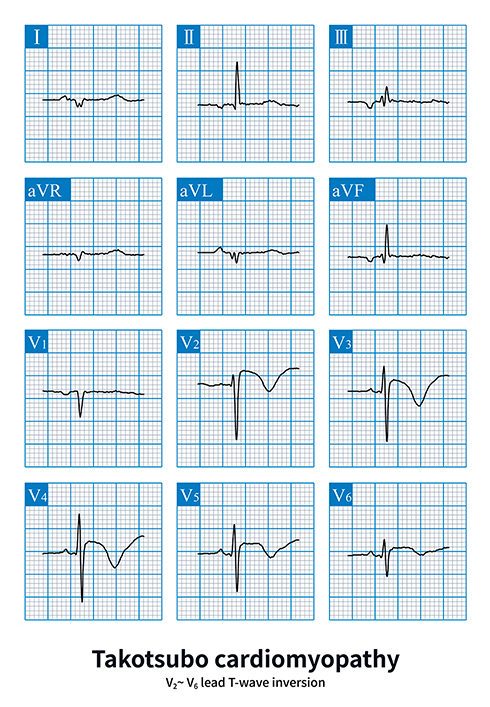
While Takotsubo cardiomyopathy’s cause is believed to be stress-related, researchers are still investigating the exact mechanism. It may be that the stress triggers an acute inflammation of the heart tissue.
Sebagian besar pasien akan mulai pulih secara spontan dalam beberapa jam hingga beberapa hari, tetapi otot jantung membutuhkan waktu lebih lama untuk pulih. Sebuah studi tahun 2018 oleh Aberdeen University menemukan tanda-tanda berkurangnya peradangan lima bulan setelah episode Takotsubo. Peradangan ini dapat menyebabkan gejala jangka panjang, termasuk kelelahan, nyeri dada, dan kekurangan energi.
Informasi yang kami miliki menunjukkan peluang 10 hingga 15 persen untuk kambuh, meskipun pemicunya mungkin berbeda. Kekambuhan saat berada di bawah air dapat berakibat fatal.
Menentukan kebugaran Anda untuk kembali menyelam sama seperti penyelam dengan kondisi jantung yang signifikan, yang semuanya berdasarkan kasus per kasus. Kesehatan Anda secara keseluruhan dan kemampuan Anda untuk berolahraga tanpa merasa lemah, lelah, atau sesak napas merupakan bagian dari hal tersebut, demikian pula obat apa pun yang Anda minum dan riwayat medis Anda yang lain.
Kami merekomendasikan tindak lanjut yang cermat dengan ahli jantung Anda selama masa pemulihan dan menunggu untuk memastikan bahwa Anda benar-benar bebas dari gejala dan toleransi olahraga Anda telah kembali normal sebelum mempertimbangkan untuk kembali menyelam. Kemudian Anda harus berbicara dengan ahli jantung Anda tentang keinginan Anda untuk menyelam, menjalani kebugaran fisik yang lengkap untuk menyelam, dan memahami implikasi serius jika gejala kambuh saat menyelam.
Angka kematian di rumah sakit, rawat inap untuk gangguan stres, dan rawat inap kembali untuk masalah kardiovaskular dilaporkan lebih tinggi secara signifikan dibandingkan mereka yang tidak memiliki kondisi ini.
—Robert Soncini, NR-P, DMT
© Alert Diver — Q3 2022